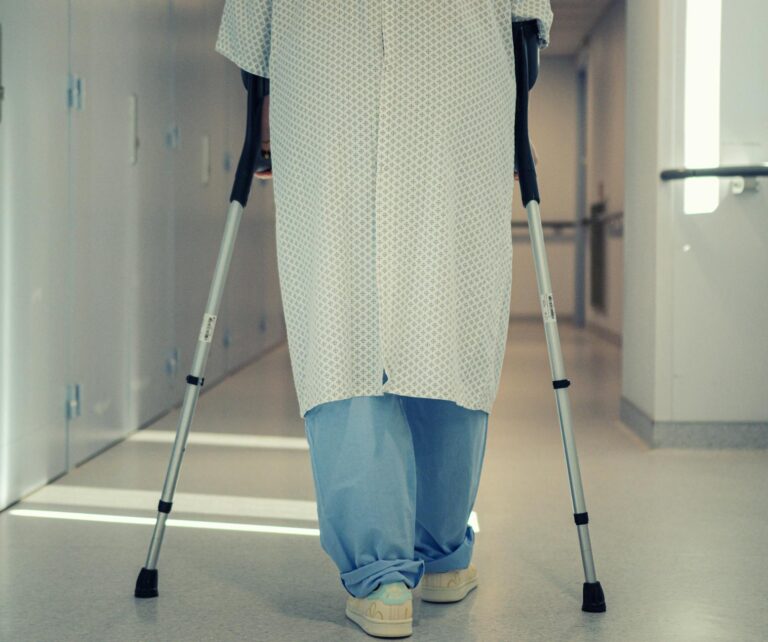
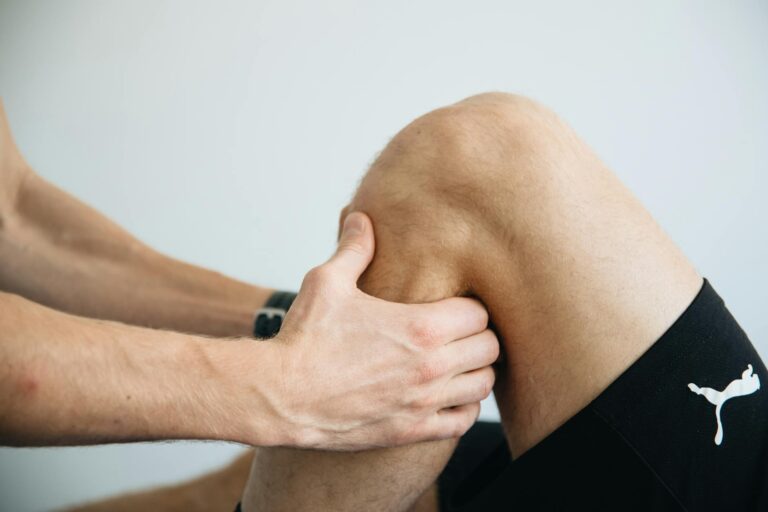
Falls are the leading cause of injury-related death in adults over 65 — and a significant hip fracture or head injury can require weeks of skilled rehabilitation before safe return home. Understanding the recovery process helps families navigate this difficult period.
Common Fall Injuries Requiring SNF Rehabilitation
- Hip fracture: The most common serious fall injury in older adults. Most hip fractures require surgical repair (ORIF or hip replacement), followed by SNF rehabilitation.
- Wrist fracture (Colles’ fracture): Common in people who put hands out to catch themselves. Usually managed with casting; OT focuses on regaining hand function.
- Vertebral compression fracture: Can cause significant pain and mobility limitation; PT focuses on pain management and safe mobility.
- Traumatic brain injury (TBI): Even a “mild” TBI in an older adult can require cognitive rehabilitation and close medical monitoring.
Hip Fracture: The Most Serious Fall Injury
Hip fractures in older adults carry a sobering prognosis: up to 30% of older adults who sustain a hip fracture die within 12 months, often from complications of immobility (pneumonia, blood clots, pressure injuries). Aggressive, early rehabilitation significantly improves outcomes.
After surgical repair, patients typically transfer to SNF within 2–5 days. Physical therapy begins almost immediately — often the day after surgery — with the goal of restoring mobility, preventing complications, and returning to independent living.

Fall Prevention: A Critical Part of Rehab
Perhaps the most important goal of rehabilitation after a fall is preventing the next one. Every SNF patient who has fallen receives a comprehensive fall risk assessment and individualized prevention plan including:

- Balance and strength training targeted at fall risk factors
- Medication review (many medications increase fall risk)
- Vision screening referral if indicated
- Footwear assessment and recommendations
- Home hazard identification (rugs, lighting, bathroom safety)
Related Resources

April 19, 2026